 Your new post is loading...
 Your new post is loading...
More than 100 million HIV tests are performed around the world annually, meaning even a small improvement in quality assurance could impact the lives of millions of people by reducing the risk of false positives and negatives. Academics from the London Center for Nanotechnology at UCL and AHRI used deep learning (artificial intelligence/AI) algorithms to improve health workers' ability to diagnose HIV using lateral flow tests in rural South Africa. Their findings, published today in Nature Medicine, involve the first and largest study of field-acquired HIV test results, which have applied machine learning (AI) to help classify them as positive or negative. By harnessing the potential of mobile phone sensors, cameras, processing power and data sharing capabilities, the team developed an app that can read test results from an image taken by end users on a mobile device. It may also be able to report results to public health systems for better data collection and ongoing care. read the study at https://www.nature.com/articles/s41591-021-01384-9 read more at https://medicalxpress.com/news/2021-06-ai-app-hiv-accurately.html
Via nrip
Adherence to treatment is critical for successful treatment outcomes. Although factors influencing antiretroviral therapy (ART) adherence vary, young adults are less likely to adhere owing to psychosocial issues such as stigma, ART-related side effects, and a lack of access to treatment. The Call for Life Uganda (CFLU) mobile health (mHealth) tool is a mobile phone–based technology that provides text messages or interactive voice response functionalities through a web interface and offers 4 modules of support.
Objective: This study aims to describe the acceptability and feasibility of a mobile phone support tool to promote adherence to ART among young adults in a randomized controlled trial.
Methods: An exploratory qualitative design with a phenomenological approach at 2 study sites was used. A total of 17 purposively selected young adults with HIV infection who had used the mHealth tool CFLU from 2 clinics were included. In total, 11 in-depth interviews and 1 focus group discussion were conducted to examine the following topics: experience with the CFLU tool (benefits and challenges), components of the tool, the efficiency of the system (level of comfort, ease, or difficulty in using the system), how CFLU resolved adherence challenges, and suggestions to improve CFLU. Participants belonged to 4 categories of interest: young adults on ART for the prevention of mother-to-child transmission, young adults switching to or on the second-line ART, positive partners in an HIV-discordant relationship, and young adults initiating the first-line ART. All young adults had 12 months of daily experience using the tool. Data were analyzed using NVivo version 11 software (QSR International Limited) based on a thematic approach.
Results: The CFLU mHealth tool was perceived as an acceptable intervention;
young adults reported improvement in medication adherence, strengthened clinician-patient relationships, and increased health knowledge from health tips. Appointment reminders and symptom reporting were singled out as beneficial and helped to address the problems of forgetfulness and stigma-related issues. HIV-related stigma was reported by a few young people. Participants requested extra support for scaling up CFLU to make it more youth friendly. Improving the tool to reduce technical issues, including network outages and a period of software failure, was suggested. They suggested that in addition to digital solutions, other support, including the promotion of peer support meetings and the establishment of a designated space and staff members for youth, was also important.
Conclusions: This mHealth tool was an acceptable and feasible strategy for improving ART adherence and retention among young adults in resource-limited settings.
read the entire study at https://mhealth.jmir.org/2021/6/e17418/
Via nrip
Atypical eye gaze is an early-emerging symptom of autism spectrum disorder (ASD) and holds promise for autism screening. Current eye-tracking methods are expensive and require special equipment and calibration. There is a need for scalable, feasible methods for measuring eye gaze. This case-control study examines whether a mobile app that displays strategically designed brief movies can elicit and quantify differences in eye-gaze patterns of toddlers with autism spectrum disorder (ASD) vs those with typical development. In effect, using computational methods based on computer vision analysis, can a smartphone or tablet be used in real-world settings to reliably detect early symptoms of autism spectrum disorder? Findings In this study, a mobile device application deployed on a smartphone or tablet and used during a pediatric visit detected distinctive eye-gaze patterns in toddlers with autism spectrum disorder compared with typically developing toddlers, which were characterized by reduced attention to social stimuli and deficits in coordinating gaze with speech sounds. What this means These methods may have potential for developing scalable autism screening tools, exportable to natural settings, and enabling data sets amenable to machine learning. Conclusions and Relevance The app reliably measured both known and new gaze biomarkers that distinguished toddlers with ASD vs typical development. These novel results may have potential for developing scalable autism screening tools, exportable to natural settings, and enabling data sets amenable to machine learning. read the study at https://jamanetwork.com/journals/jamapediatrics/fullarticle/2779395
Lire l'article complet sur : jamanetwork.com
Via nrip
The app incorporates CBT to improve high relapse rates
Via Rémy TESTON
Consumers are looking to mobile health tools, such as mHealth apps and wearables, to improve their medication adherence. A recent study of some 800 prescription medication users, conducted by Russell Research for Express Scripts, finds that roughly half believe mHealth technology would help them become more adherent – and one-third of those would be more likely to use them if the tools were set up for them. With experts suggesting at least half of the nation’s medication users aren’t taking their drugs as prescribed – costing some $300 billion a year in avoidable healthcare expenses, or $1,000 per person – medication adherence is a significant issue and one that healthcare experts have vowed to tackle more aggressively. “This survey shows that while patients with chronic diseases know that medication is critical to their treatment and health, they don’t always act on that knowledge,” Snezana Mahon, PharmD, vice president of St. Louis-based Express Scripts Clinical Solutions, said in a press release. “Given the huge cost of nonadherence to an individual patient’s health, as well as to the country as a whole, it’s essential for patients and clinicians to work together to find solutions to help overcome barriers to adherence.” Those taking medications would seem to agree. Almost half of those surveyed said taking their drugs as prescribed is the most important part of their health regimen, a percentage higher than those selecting a routine check-up (30 percent). And they seem interested in improving their habits: 56 percent said reminders would more likely help them improve adherence, and 19 percent said those reminders would definitely help them. That’s where mHealth comes in. “The three main drivers of non-adherence come from cost, clinical or behavioral reasons,” said Kyle Amelung, PharmD, BCPS, a senior clinical consultant on Express Scripts. “All three can be solved for through mobile health tools.” Younger consumers are particularly interested in mobile health technology: 74 percent of those between the ages of 18 and 34 believe such tools would help them, and half would be more likely to use the technology if it was set up for them. Among those age 35-54, the percentages were 62 and 46, respectively. “We believe success comes from getting within the patient’s flow and reminding them about their health when and how the patient prefers,” Amelung said. “Most people view mobile devices as a personal productivity tool that can be used to check the news, connect with friends or get the score of the game. Incorporating these devices into taking better care of yourself is a logical position – but people still don’t want to be ‘nagged’ by family or friends about their health.” That point was also made in the survey: 27 percent said they would most not want to be reminded to take their medications by a health device, while 40 percent said a spouse or partner would be most bothersome and 31 percent said the same of a friend. In each case, respondents felt that they’d be nagged by those prods and end up resenting the reminders. Amelung emphasized that mHealth alone won’t solve the medication adherence issue. “The key to mHealth tools is partnering them with a live clinician that can oversee the data, flag high-risk patients, and intervene as appropriate,” he said. “Technology is not the solution; technology is the means to an effective solution. To truly affect change, any proposed solution must be partnered with live clinical support to answer any questions and provide specialized guidance to the patient.” The survey also shed some interesting light on prescription habits. More than half of those surveyed feel they’re doing better at sticking to their prescriptions than others – including 60 percent of seniors. And more respondents were unconcerned about missing a medication (31 percent) than were extremely or very concerned (29 percent). Among other results: - 67 percent would be motivated by a reward to take their medications as prescribed.
- 82 percent would be motivated to take their medications by a financial reward, while 15 percent chose points toward a merchandise purchase and 3 percent selected a charitable contribution.
- Only 33 percent understand the financial significance of medication adherence; 35 percent believe the annual cost to healthcare runs about $150 billion (or $500 per person), while 19 percent put that figure at $25 billion ($75 per person) and 12 percent said the cost was around $8.3 billion, or $25 per person.
- 44 percent cited side effects as the primary reason for not taking medications as prescribed; 28 percent picked inconvenience and 21 percent said they stopped taking their drugs because they were feeling better and felt they didn’t need to continue the prescription.
Amelung said some of the survey’s results surprised him. “One of the most surprising findings was that two-thirds of those polled say they are more likely to take better care of their health and adhere to their medications when rewarded for their efforts,” he noted. “We all want to be in optimal health, but this data point supports the long-standing belief that only the potential of better health outcomes is not sufficient in getting patients to make the best decisions and take the appropriate actions for their health.” “In today’s world, the distractions of the moment often get in the way of pursuing what’s in the best interest of our care. We sometimes forgo scheduling or keeping doctor appointments. We skip necessary lab tests or our annual flu shot. Many of us forget to refill our medication or we don’t remember to take it every day. … For most of us, engaging in the right daily behaviors to improve our health is a challenge because these actions fall out of our normal routines and habits – and so, we skip them. Knowing that there must be something more for the patient to obtain and that financial rewards are an effective way to motivate patients, we can offer specific carrots to incentivize healthier actions and lead to decrease costs in the healthcare system.”
mHealth is now entering the mainstream consciousness and the pace of innovation is rapid with new breakthroughs announced on a daily basis.
Via Bruno Demay
82 % des organismes qui délivrent des soins de santé (mHealth) interrogés dans une étude pour RedHat ont une stratégie full mobile, indiquant un niveau de maturité plus élevé
A survey conducted by Nielsen on behalf of the Council of Accountable Physician Practices (CAPP) finds that, at most, 52 percent of primary care physicians have recommended that their patients use an mHealth app or device to track their health. Yet only 4 percent to 5 percent of consumers surveyed say their PCP has made such a recommendation. This means that either physicians are making the effort but their patients are ignoring the advice, or patients are looking for that guidance but it isn’t coming from their doctors. The survey reached a familiar conclusion in how each generation perceives mHealth and telehealth. It found that consumers rarely use video visits (only 5 percent total), but those age 34 and younger are twice as likely to use and want them than those age 65 and older. The same discrepancy was seen in the use of text reminders for medication and health measurements and online scheduling tools. more at : http://mhealthintelligence.com/news/do-doctors-patients-take-mhealth-seriously
Via nrip, Pharma Guy
The market of mobile health (mHealth) apps has rapidly evolved in the past decade. With more than 100,000 mHealth apps currently available, there is no centralized resource that collects information on these health-related apps for researchers in this field to effectively evaluate the strength and weakness of these apps. Objective The objective of this study was to create a centralized mHealth app repository. We expect the analysis of information in this repository to provide insights for future mHealth research developments. Methods We focused on apps from the two most established app stores, the Apple App Store and the Google Play Store. We extracted detailed information of each health-related app from these two app stores via our python crawling program, and then stored the information in both a user-friendly array format and a standard JavaScript Object Notation (JSON) format. Results We have developed a centralized resource that provides detailed information of more than 60,000 health-related apps from the Apple App Store and the Google Play Store. Using this information resource, we analyzed thousands of apps systematically and provide an overview of the trends for mHealth apps. Conclusions This unique database allows the meta-analysis of health-related apps and provides guidance for research designs of future apps in the mHealth field.
Via nrip
It’s hard to find a pharma or medical device company these days that doesn’t have at least one mobile app in development. And now that, as of February 2015, the U.S. Food and Drug Administration (FDA) has issued guidance on which apps need to be regulated and which ones don’t, it will be interesting to see if this almost exponential development trend continues.
Federal guidance alone doesn’t guarantee an app’s success, and there is still plenty of playing field for developers in the health and wellness space for apps that do not require 510(k) submission. Therefore, developers and marketers alike must keep in mind these three key drivers of mobile health app adoption.
Awareness In a 2014 poll by QuantiaMD, only 37% of physicians surveyed said that they had recommended a mobile app to their patients. In another QuantiaMD poll, 42% of physicians said they would notrecommend a mobile health app to patients because there was no regulatory oversight (though the new FDA guidance should help with this). In addition, another 37% percent had no idea what mobile health apps are out there.
In spite of physicians being split on the utility of apps, consumers are downloading them at a rapid pace. In fact, it is estimated that within the next three years half of all smartphone and tablet users will have at least one mobile health or wellness app, like Lose It!, RunKeeper, or Glucose Buddy. But, downloading doesn’t necessarily mean they are using them! There is enormous opportunity for healthcare marketers to more effectively demonstrate the myriad of app benefits to patients and physicians alike.
More here...
Via Pharma Guy, Giuseppe Fattori
|
Researchers have figured out a way to use images from a smartphone to identify potentially harmful bacteria on the skin and in the mouth. A new method that uses smartphone-derived images can identify potentially harmful bacteria on the skin and in the mouth, research shows. The approach can visually identify microbes on skin contributing to acne and slow wound healing, as well as bacteria in the oral cavity that can cause gingivitis and dental plaques. Researchers combined a smartphone-case modification with image-processing methods to illuminate bacteria on images taken by a conventional smartphone camera. This approach yielded a relatively low-cost and quick method that could be used at home. The team augmented a smartphone camera’s capabilities by attaching a small 3D-printed ring containing 10 LED black lights around a smartphone case’s camera opening. The researchers used the LED-augmented smartphone to take images of the oral cavity and skin on the face of two research subjects. The LED lights ‘excite’ a class of bacteria-derived molecules called porphyrins, causing them to emit a red fluorescent signal that the smartphone camera can then pick up Other components in the image—such as proteins or oily molecules our bodies produce, as well as skin, teeth, and gums—won’t glow red under LED. They’ll fluoresce in other colors. The LED illumination gave the team enough visual information to computationally “convert” the RGB colors from the smartphone-derived images into other wavelengths in the visual spectrum. This generates a “pseudo-multispectral” image consisting of 15 different sections of the visual spectrum—rather than the three in the original RGB image. Obtaining this visual information up front would have required expensive and cumbersome lights, rather than using the relatively inexpensive LED black lights With their greater degree of visual discrimination, the pseudo-multispectral images clearly resolved porphyrin clusters on the skin and within the oral cavity. In addition, though they tailored this method to show porphyrin, researchers could modify the image-analysis pipeline to detect other bacterial signatures that also fluoresce under LED. read the study at https://doi.org/10.1016/j.optlaseng.2021.106546 read the original unedited article at https://www.futurity.org/smartphone-images-skin-mouth-bacteria-2581642/
Via nrip
Mobile health apps are becoming increasingly popular, and they provide opportunities for effective health management. Existing chronic disease management (CDM) apps cannot meet users’ practical and urgent needs, and user adhesion is poor. Few studies, however, have investigated the factors that influence the continuance intention of CDM app users. Objective: Starting from the affordances of CDM apps, this study aimed to analyze how such apps can influence continuance intention through the role of health empowerment. Methods: Adopting a stimulus-organism-response framework, an antecedent model was established for continuance intention from the perspective of perceived affordances, uses and gratifications theory, and health empowerment. Perceived affordances were used as the “stimulus,” users’ gratifications and health empowerment were used as the “organism,” and continuance intention was used as the “response.” Data were collected online through a well-known questionnaire survey platform in China, and 323 valid questionnaires were obtained. The theoretical model was tested using structural equation modeling. Results: Perceived connection affordances were found to have significant positive effects on social interactivity gratification (t717=6.201, P<.001) and informativeness gratification (t717=5.068, P<.001). Perceived utilitarian affordances had significant positive effects - on informativeness gratification (t717=7.029, P<.001),
- technology gratification (t717=8.404, P<.001),
- and function gratification (t717=9.812, P<.001).
Perceived hedonic affordances had - significant positive effects on function gratification (t717=5.305, P<.001)
- and enjoyment gratification (t717=13.768, P<.001).
Five gratifications (t717=2.767, P=.005; t717=4.632, P<.001; t717=7.608, P<.001; t717=2.496, P=.012; t717=5.088, P<.001) had significant positive effects on health empowerment. Social interactivity gratification, informativeness gratification, and function gratification had significant positive effects on continuance intention. Technology gratification and enjoyment gratification did not have a significant effect on continuance intention. Health empowerment had a significant positive effect on continuance intention. Health empowerment and gratifications play mediating roles in the influence of affordances on continuance intention. Conclusions: Health empowerment and gratifications of users’ needs are effective ways to promote continuance intention. The gratifications of users’ needs can realize health empowerment and then inspire continuance intention. Affordances are key antecedents that affect gratifications of users’ needs, health empowerment, and continuance intention. The results indicated that users’ perceptions of an app’s affordances can promote the gratification of needs, and the gratification of key needs (ie, social interactivity, informativeness, technology, and function gratification) can stimulate users’ continuance intention. At the same time, the gratification of users’ needs can promote users’ cognitions of health empowerment, thus stimulating continuance intention. Health empowerment was found to play a mediating role in the influence of gratification on continuance intention. From a practical perspective, app service providers should design apps from the perspective of social interaction (eg, providing social networks), utilitarian functions (eg, health self-management), and hedonic functions (eg, enhancing the user’s interest). By meeting users’ various needs, app developers can improve the user’s ability to control his or her own health, thus achieving the purpose of extending the life of the app. more at https://mhealth.jmir.org/2021/5/e21831/
Lire l'article complet sur : mhealth.jmir.org
Via nrip
The American Health Information Management Association is giving providers a resource site for evaluating digital health tools, and giving mHealth vendors an opportunity to seek AHIMA certification. AHIMA has unveiled AHIMA dHealth, a site which offers resources for healthcare providers on digital health products, including privacy and data security practices and policies, and an assessment tool designed to help vendors meet AHIMA standards. To become AHIMA-certified, a vendor will have to complete a self-reported assessment based on the organization’s standards and best practices for privacy and security. As per the CEO of AHIMA, “Earning AHIMA dHealth Approval shows that your product takes privacy and data security seriously, Having this designation allows developers to build trust with providers and patients, which has the potential to earn and positively impact more users.” CVS Health is also giving the digital health industry some love. The company has launched a $100 million venture capital fund targeting early-stage companies that are developing “cutting-edge, digitally enabled solutions.” to learn more read the entire article at https://mhealthintelligence.com/news/ahima-launches-mhealth-resource-assessment-tool-for-vendors
Lire l'article complet sur : mhealthintelligence.com
Via nrip
Healthcare providers who access clinical decision support through mHealth platforms are finding a world of information at their fingertips – and they could be saving lives. Digital technologies are changing the way medical information is gathered and exchanged. Physicians of all ages and medical subspecialties from across the globe are utilizing tools to discuss potential diagnoses and obtain second opinions. That’s the takeaway from researchers at the Scripps Research Translational Institute who took a closer look at online crowdsourced consult platforms. Their conclusion is that these platforms, which include social media networks like SERMO, Medscape and HealthTap, are giving providers quick access to information that’s helping them reduce serious, costly and potentially deadly medical errors. The study, focusing on an analysis of more than 37,000 active users on the MedScape Consult network between 2015 and 2017, appears in a recent issue of NPJ Digital Medicine. The research points to the value of a mobile health resource for clinical decision support, giving providers a real-time portal for physician-to-physician engagement. Billed as a source for “the second to hundredth opinion in medicine,” these portals allow providers to gather best practices and apply them quickly, reducing the chances of a clinical error. The study also points to the changing nature of clinical decision support.The study noted that providers can’t necessarily rely on informal face-to-face consults with colleagues – commonly known as curbside consults – because they’re “frequently inaccurate and incomplete.” Yet they can’t just call up a nearby specialist at a moment’s notice. The study found that : "At a time when we’re turning to artificial intelligence to help improve diagnostic accuracy, there’s still plenty of room for tapping into human intelligence via such medical consulting platforms, Artificial intelligence has been advocated as the definitive pathway for reducing misdiagnosis, But the study's findings suggest the potential for collective human intelligence, which is algorithm-free and performed rapidly on a voluntary basis, to emerge as a competitive or complementary strategy."
Via nrip
In order to envisage a better (i.e. more transparent, safe, accessible, sustainable and efficient) health system than we have today, we must lift our vision above the siloed mobile health app as the building block of future improvement. Seen correctly, mobile apps are the current delivery channel of choice for new, digitally-enabled models of care, but not …
Researchers enlist smartphones and machine learning to find vocal patterns that might signal post-traumatic stress disorder or even heart disease.
Via Julie O'Donnell
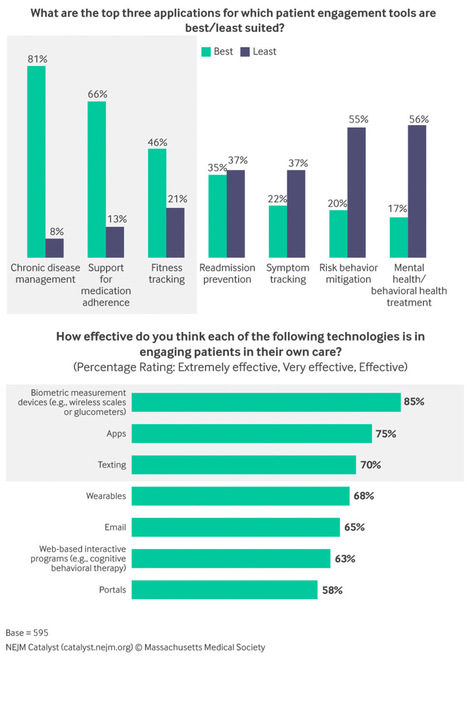
Healthcare providers see patient engagement tools as a means of better understanding each patient’s overall health and offering new pathways for predictive analytics, but many are still hesitant to steer patients towards certain technology. More than two-thirds of respondents said technology can help support healthy behaviors among patients, according to a survey released by NEJM Catalyst. More than half said technology generates additional data for analytics. But 67% of respondents also said they don’t know what tools to recommend to patients, and 42% said it’s still unclear how tools actually impact care. Biometric devices, mHealth apps and texting were identified as the most effective patient engagement tools. Eighty-one percent of respondents said these tools were best used to manage chronic diseases. For example, a new online tool recently released by Anthem aims to help providers and patients better understand gaps in asthma care. Further Reading: - “AMA Survey Finds That Many Physicians Are Enthusiastic About Digital Health Tools, But Few Currently Use Them”; http://sco.lt/8b9r97
- “Six Top Global Pharma Companies Establish New HCP Technology Standards Group”; http://sco.lt/820SMj
Via Pharma Guy
The results of this year’s mHealth App Developer Economics 2016 study show a steep increase in competition level among mHealth app publishers. The supply side of mHealth apps is measured in the number of available apps and publishers. They are growing significantly faster than the demand side which is quantified by the number of mHealth app downloads. The number of mHealth apps and active mHealth app publishers has seen strong growth since 2015. This year, the total number of mHealth apps listed on major app stores across the globe grew by 57% to 259,000 apps. This impressive growth is based on three main developments; the growing number of mHealth app publishers, the increased importance of multi-platform app publishing and the expansion of existing mHealth app portfolios. The number of mHealth app publishers grew in line with the number of apps. There are currently 58,000 mHealth app publishers app on major app stores, 28% more since the beginning of 2015. There appears to be no immediate end to the number of companies rushing into the market to launch their first mHealth app. In contrast, growth rates of mHealth app store downloads are estimated to be only +7% in 2016, having been +35% the previous year, reaching a total of 3.2B in 2016. This is in line with other app market categories and reflects the fact that growth of capable devices that can download apps has slowed down in most western countries. As a consequence of this increased competition, it will be even more difficult to stand out and gain significant downloads. Only 14% of mHealth app publishers generated more than 100,000 downloads with their mHealth app portfolio in one year. With hundreds of new mHealth apps released daily, companies have to consider their app launch as if it were a familiar product in a saturated market.
Via Pharma Guy, Giuseppe Fattori
You’re developing a health app for mobile devices and you want to know which federal laws apply. Check out this interactive tool.
WHAT ARE THE LAWS?
Does your mobile app collect, create, or share consumer information? Does it diagnose or treat a disease or health condition? Then this tool will help you figure out which – and it may be more than one – federal laws apply. It’s not meant to be legal advice about all of your compliance obligations, but it will give you a snapshot of a few important laws and regulations from three federal agencies.
- Health Insurance Portability and Accountability Act (HIPAA)
- Federal Food, Drug, and Cosmetic Act (FD&C Act)
- Federal Trade Commission Act (FTC Act)
- FTC’s Health Breach Notification Rule
WHICH LAWS APPLY TO YOUR MOBILE HEALTH APP? Go here.
Via Pharma Guy, Giuseppe Fattori
Mobile phones with operating systems and capable of running applications (smartphones) are increasingly being used in clinical settings. Medical calculating applications are popular mhealth apps for smartphones. These include, for example, apps that calculate the severity or likelihood of disease-based clinical scoring systems, such as determining the severity of liver disease, the likelihood of having a pulmonary embolism, and risk stratification in acute coronary syndrome. However, the accuracy of these apps has not been assessed. OBJECTIVE: The objective of this study was to evaluate the accuracy of smartphone-based medical calculation apps.
CONCLUSIONS: The results suggest that most medical calculating apps provide accurate and reliable results. The free apps that were 100% accurate and contained the most functions desired by internists were CliniCalc, Calculate by QxMD, and Medscape. When using medical calculating apps, the answers will likely be accurate; however, it is important to be careful when calculating MELD scores or Child-Pugh scores on some apps. Despite the few errors found, greater scrutiny is warranted to ensure full accuracy of smartphone medical calculator apps.
Via nrip
HealthTap published a survey of the top physician-rated apps for both iOS and Android, and breaks it down into 30 separate categories. HealthTap founder and CEO Ron Gutman said the company's goal is to give clinicians and consumers a guide to choosing apps that have been approved by doctors, rather than resorting to the user ratings found in app stores (HealthTap's AppRx app, by the way, has a healthy 4.72 star rating in the Apple App Store, he said). The apps are judged on three standards – ease of use, effectiveness and medical accuracy, validity and soundness. They're not given a number rating, but are ranked solely based on how many doctors would recommend them. Top 10 Health and Medical Apps for Android 1. Weight Watchers Mobile (Weight Watchers International) 2. White Noise Lite (TMSoft) 3. Lose It! (FitNow) 4. First Aid (American Red Cross) 5. RunKeeper – GPS Track Run Walk (FitnessKeeper) 6. Emergency First Aid/Treatment (Phoneflips) 7. Instant Heart Rate (Azumio) 8. Fooducate – Healthy Food Diet (Fooducate) 9. Glucose Buddy – Diabetes Log (Azumio) 10. Pocket First Aid & CPR (Jive Media) Top Health and Medical Apps for iOS 1. Calorie Counter and Diet Tracker (MyFitnessPal.com) 2. Weight Watchers Mobile (Weight Watchers International) 3. Lose It! (FitNow) 4. White Noise Lite (TMSoft) 5. First Aid (American Red Cross) 6. Runkeeper (FitnessKeeper) 7. Stroke Riskometer (Autel) 8. Emergency First Aid & Treatment Guide (Phoneflips) 9. Instant Heart Rate (Azumio) 10. Fooducate (Foducate) more at http://www.mhealthnews.com/news/top-mhealth-apps-rated-doctors?single-page=true
Via nrip, nancygabor
|



 Your new post is loading...
Your new post is loading...
































The use of mobile tools for data capture and AI/ML algorithms for diagnostics and detections has been the inside story of digital health over the past 4 years. This is an excellent study and shows the promise of this combination of technologies in building the future of healthcare. HIV is a pandemic which must be eradicated.