Your new post is loading...
 Your new post is loading...

|
Scooped by
AXELIFE
|
Many studies found that increased arterial stiffness is significantly associated with the presence and progression of Coronary Calcium Score (CCS). However, none so far have used machine learning algorithms to improve their value. Therefore, this stud

|
Scooped by
AXELIFE
|
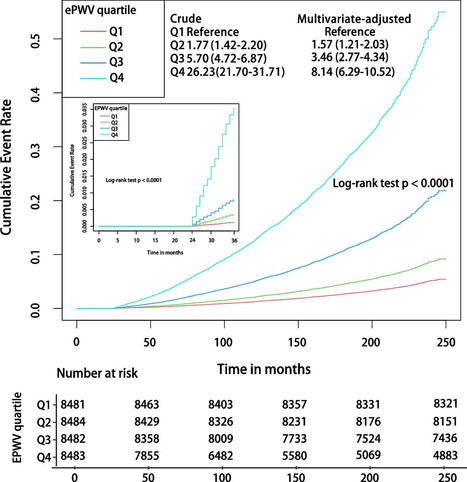
Background Estimated pulse wave velocity (ePWV) has been proposed as a potential approach to estimate carotid-femoral pulse wave velocity. However, the potential of ePWV in predicting all-cause mortality (ACM) and cardiovascular disease mortality (CVM) in the general population is unclear. Methods We conducted a prospective cohort study using the data of 33,930 adults (age ≥ 20 years) from the National Health and Nutrition Examination Survey (NHANES) from 1999 to 2014 until the end of December 2019. The study outcomes included ACM and CVM. Survey-weighted Cox proportional hazards models were used to assess hazard ratios (HRs) and 95% confidence intervals (CIs) to determine the association between ePWV and ACM and CVM. To further investigate whether ePWV was superior to traditional risk factors in predicting ACM and CVM, comparisons between ePWV and the Framingham Risk Score (FRS) and Pooled Cohort Equations (PCE) models were performed. Integrated Discriminant Improvement (IDI) and Net Reclassification Improvement (NRI) were employed to analyze differences in predictive ability between models. Results The weighted mean age of the 33,930 adults included was 45.2 years, and 50.28% of all participants were men. In the fully adjusted Cox regression model, each 1 m/s increase in ePWV was associated with 50% and 49% increases in the risk of ACM (HR 1.50; 95% CI, 1.45–1.54) and CVM (HR 1.49; 95% CI, 1.41–1.57), respectively. After adjusting for FRS, each 1 m/s increase in ePWV was still associated with 29% (HR 1.29; 95% CI, 1.24–1.34) and 34% (HR 1.34; 95% CI, 1.23–1.45) increases in the risk of ACM and CVM, respectively. The area under the curve (AUC) predicted by ePWV for 10-year ACM and CVM were 0.822 and 0.835, respectively. Compared with the FRS model, the ePWV model improved the predictive value of ACM and CVM by 5.1% and 3.8%, respectively, with no further improvement in event classification. In comparison with the PCE model, the ePWV model’s ability to predict 10-year ACM and CVM was improved by 5.1% and 3.5%, and event classification improvement was improved by 34.5% and 37.4%. Conclusions In the U.S. adults, ePWV is an independent risk factor for ACM and CVM and is independent of traditional risk factors. In the general population aged 20 to 85 years, ePWV has a robust predictive value for the risk of ACM and CVM, superior to the FRS and PCE models. The predictive power of ePWV likely originates from the traditional risk factors incorporated into its calculation, rather than from an indirect association with measured pulse wave velocity.

|
Scooped by
AXELIFE
|
The automated detection of induced circulatory arrests using wrist-derived photoplethysmography
is feasible with good sensitivity and low false positives. These promising findings
warrant further development of this wearable technology to enable automated cardiac
arrest detection and alarming in a home setting.

|
Scooped by
AXELIFE
|
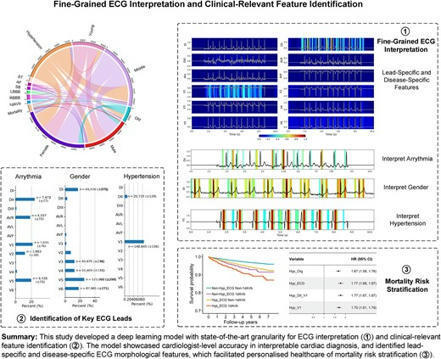
AbstractAims. Electrocardiogram (ECG) is widely considered the primary test for evaluating cardiovascular diseases. However, the use of artificial intellig

|
Scooped by
AXELIFE
|
A new study published in JAMA Open Network finds that digital health interventions can help reduce blood pressure when used in populations experiencing health

|
Scooped by
AXELIFE
|
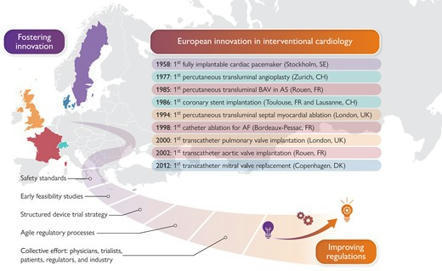
Abstract. Research performed in Europe has driven cardiovascular device innovation. This includes, but is not limited to, percutaneous coronary intervention, ca

|
Scooped by
AXELIFE
|
NYU Grossman School of Medicine researchers used artificial intelligence and wearable activity trackers to improve the monitoring and classification of older adult cardiac rehabilitation patients.

|
Scooped by
AXELIFE
|
Research shows digital health interventions positively impacted hypertension control among vulnerable patients, including low-income and minority race groups.

|
Scooped by
AXELIFE
|
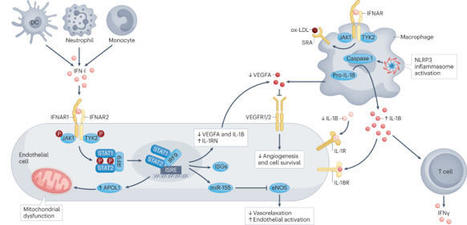
Vascular disease is a major cause of morbidity and mortality in patients with systemic autoimmune diseases, particularly systemic lupus erythematosus (SLE). Although comorbid cardiovascular risk factors are frequently present in patients with SLE, they do not explain the high burden of premature vascular disease. Profound innate and adaptive immune dysregulation seems to be the primary driver of accelerated vascular damage in SLE. In particular, evidence suggests that dysregulation of type 1 interferon (IFN-I) and aberrant neutrophils have key roles in the pathogenesis of vascular damage. IFN-I promotes endothelial dysfunction directly via effects on endothelial cells and indirectly via priming of immune cells that contribute to vascular damage. SLE neutrophils are vasculopathic in part because of their increased ability to form immunostimulatory neutrophil extracellular traps. Despite improvements in clinical care, cardiovascular disease remains the leading cause of mortality among patients with SLE, and treatments that improve vascular outcomes are urgently needed. Improved understanding of the mechanisms of vascular injury in inflammatory conditions such as SLE could also have implications for common cardiovascular diseases, such as atherosclerosis and hypertension, and may ultimately lead to personalized therapeutic approaches to the prevention and treatment of this potentially fatal complication. Here, the authors review traditional and disease-specific risk factors for vascular damage and the cellular and molecular mechanisms that drive vascular injury in systemic lupus erythematosus. They also discuss cardiovascular risk assessment, primary prevention strategies and current and future treatment approaches to cardiovascular disease in systemic lupus erythematosus.

|
Scooped by
AXELIFE
|
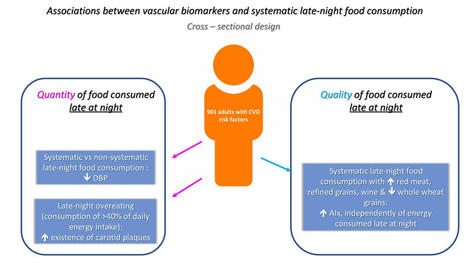
A study from the University of Gothenburg reveals significant health risks associated with staying awake late into the night, including a 90% higher risk of arterial stiffness.

|
Scooped by
AXELIFE
|
An analysis shows digital health interventions can improve stroke prevention, but due to a lack of diversity, their efficacy among minority groups is uncertain.

|
Scooped by
AXELIFE
|
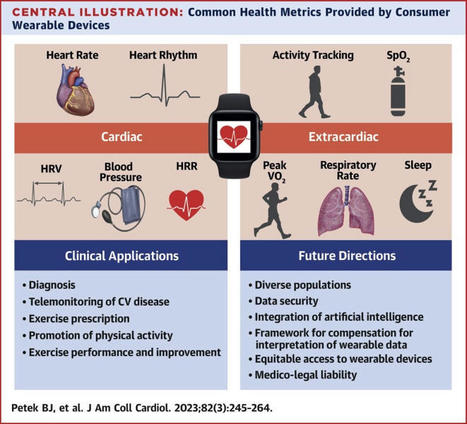
The use of consumer wearable devices (CWDs) to track health and fitness has rapidly expanded over recent years because of advances in technology. The …

|
Scooped by
AXELIFE
|
Wearable devices, such as smartwatches and activity trackers, are commonly used by patients in their everyday lives to manage their health and well-being. These devices collect and analyz
|

|
Scooped by
AXELIFE
|
In this cross-sectional study, we evaluated the completeness, readability, and syntactic complexity of cardiovascular disease prevention information produced by GPT-4 in response to 4 kinds of prompts.

|
Scooped by
AXELIFE
|
A new eye-tracking smartphone app can help detect strokes with non-specific symptoms, like dizziness, enabling more timely and effective stroke care.

|
Scooped by
AXELIFE
|
Sudden cardiac death is the cause of nearly 50% of all cardiovascular deaths and is
often precipitated by sudden cardiac arrest.1 When cardiac arrest occurs outside of
the hospital setting, it has a 9·1% survival rate to hospital discharge in the USA.1
Because there is a nearly 18% decrease in survival for every minute of delay in defibrillation,2
early detection and response to sudden cardiac arrest can mean the difference between
life and death. However, a detection technology that fits into daily life, and yet
provides accurate and actionable information, is a crucial unmet clinical need.

|
Scooped by
AXELIFE
|
Some smartwatches and fitness trackers are starting to take blood pressure readings, but the technology isn't fully developed.

|
Scooped by
AXELIFE
|
Vascular diseases, such as atherosclerosis and thrombosis, are major causes of morbidity and mortality worldwide. Traditional in vitro models for studying vascular diseases have limitations, a

|
Scooped by
AXELIFE
|
A new study published in JAMA Open Network finds that digital health interventions can help reduce blood pressure when used in populations experiencing health

|
Scooped by
AXELIFE
|
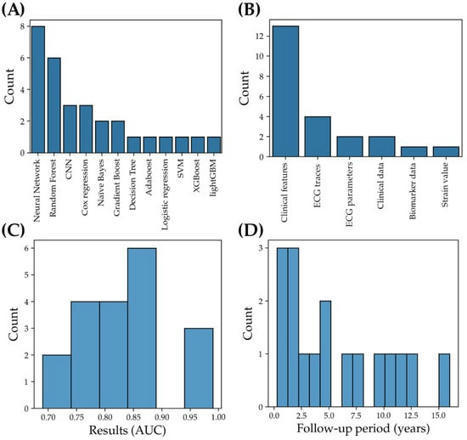
(1) Background: Atrial fibrillation (AF) is a major risk factor for stroke and is often underdiagnosed, despite being present in 13–26% of ischemic stroke patients. Recently, a significant number of machine learning (ML)-based models have been proposed for AF prediction and detection for primary and secondary stroke prevention. However, clinical translation of these technological innovations to close the AF care gap has been scant. Herein, we sought to systematically examine studies, employing ML models to predict incident AF in a population without prior AF or to detect paroxysmal AF in stroke cohorts to identify key reasons for the lack of translation into the clinical workflow. We conclude with a set of recommendations to improve the clinical translatability of ML-based models for AF. (2) Methods: MEDLINE, Embase, Web of Science, Clinicaltrials.gov, and ICTRP databases were searched for relevant articles from the inception of the databases up to September 2022 to identify peer-reviewed articles in English that used ML methods to predict incident AF or detect AF after stroke and reported adequate performance metrics. The search yielded 2815 articles, of which 16 studies using ML models to predict incident AF and three studies focusing on ML models to detect AF post-stroke were included. (3) Conclusions: This study highlights that (1) many models utilized only a limited subset of variables available from patients’ health records; (2) only 37% of models were externally validated, and stratified analysis was often lacking; (3) 0% of models and 53% of datasets were explicitly made available, limiting reproducibility and transparency; and (4) data pre-processing did not include bias mitigation and sufficient details, leading to potential selection bias. Low generalizability, high false alarm rate, and lack of interpretability were identified as additional factors to be addressed before ML models can be widely deployed in the clinical care setting. Given these limitations, our recommendations to improve the uptake of ML models for better AF outcomes include improving generalizability, reducing potential systemic biases, and investing in external validation studies whilst developing a transparent modeling pipeline to ensure reproducibility.

|
Scooped by
AXELIFE
|
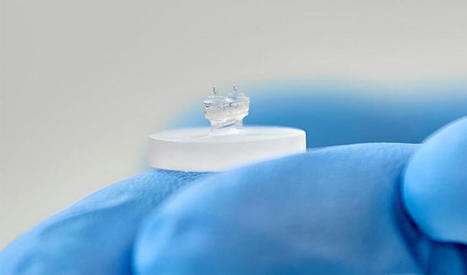
En ayant recours à la bio-impression 3D, des chercheurs ont créé un dispositif pour mieux comprendre le comportement du coeur

|
Scooped by
AXELIFE
|
Special efforts will need to be made to expand access to the different elements of digital health, ensuring that the digital divide does not exacerbate health disparities. As the expansion of digital health technologies continues, it is vital to increase representation of minoritized groups in all s …

|
Scooped by
AXELIFE
|
Cardiology makes up 10% of the 692 market-cleared clinical AI algorithms in the FDA’s latest update on the number of patient-facing AI now commercialized in the U.S. Experts share their thoughts on how it is being used.

|
Scooped by
AXELIFE
|
Cardiovascular disease (CVD) is a major global health problem. Living with diseases like CVD often requires long-term monitoring, for which flexible a…

|
Scooped by
AXELIFE
|
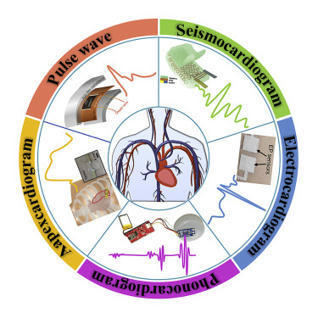
The past decade has seen a dramatic rise in consumer technologies able to monitor a variety of cardiovascular parameters. Such devices initially recor…
|
 Your new post is loading...
Your new post is loading...
 Your new post is loading...
Your new post is loading...